13point1 Advisors

How We Work
Every engagement is different. But our framework gives each one a shared language, a clear starting point, and a structured path to measurable outcomes.
The Framework

Our work is built on three layers — each one adding depth and specificity. The foundation stays constant; the application is always tailored.
Five Dimensions
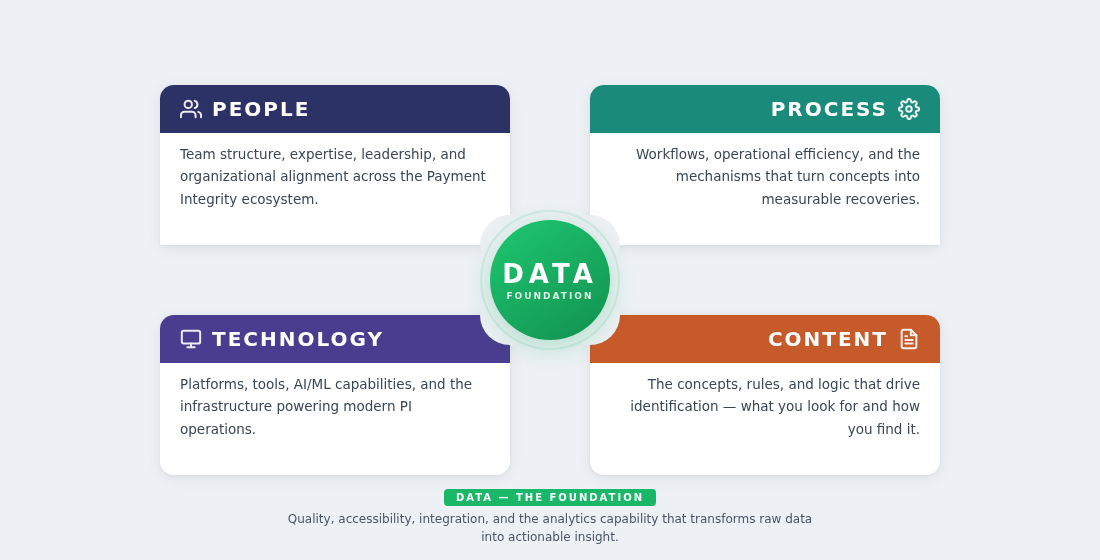
Every assessment starts here. These dimensions provide the structure to compare apples to apples — across organizations, vendors, and time.
The Reference Framework
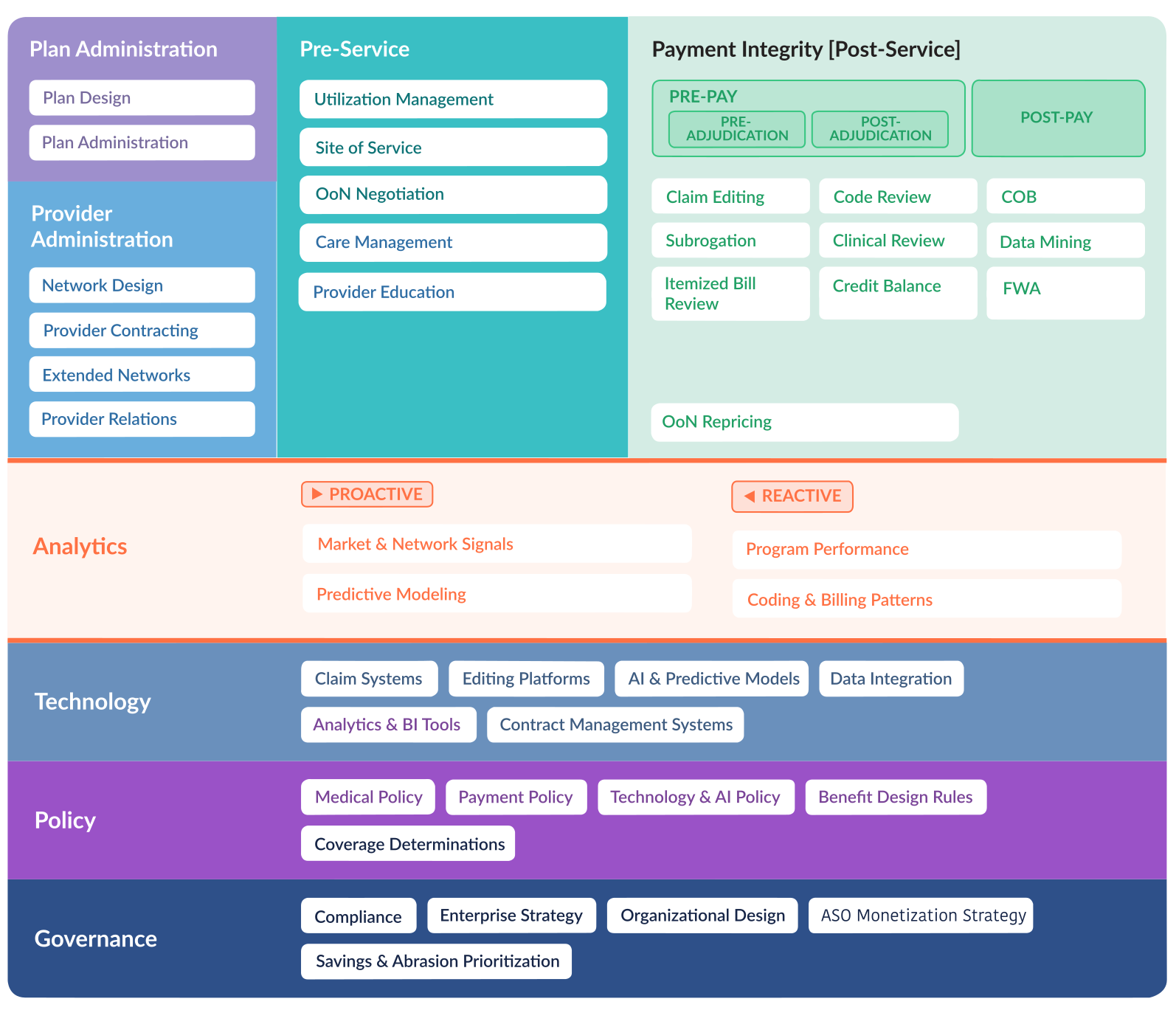
Most organizations think of Payment Integrity in isolation — a set of edits, audits, and recoveries. We see it differently. PI is one critical component within a broader cost containment ecosystem that includes plan administration, pre-service controls, provider management, analytics, technology, policy, and governance. Our Reference Framework maps the full landscape so you can see exactly where PI fits — and where the opportunities are. The ten capabilities in the upper right of the framework represent the core PI functions where we go deepest.
Pre-pay and post-pay claim edits including eligibility checks, code edits (NCCI, MUE), benefit and policy rules, duplicate detection, and clinical pends.
DRG validation, clinical validation, itemized bill review, and medical coding accuracy programs to ensure claims are paid correctly.
Coordination of Benefits — ensuring total payments across multiple health plans don't exceed 100% of allowed charges for dual-coverage members.
Third-party cost recovery for injuries or conditions with external liability — auto accidents, workers' compensation, and other liability cases.
Medical necessity and appropriateness of care reviews — ensuring clinical services meet established criteria and coverage guidelines.
Pattern-based analysis across claims data to identify overpayments, billing anomalies, and recovery opportunities at scale.
Line-by-line review of high-dollar facility claims to identify charge capture errors, unbundling, and pricing discrepancies.
Identification and resolution of negative account balances — recovering overpaid funds through credit balance programs and issue refunds.
Fraud, Waste, and Abuse — detection, prevention, investigation, and training programs that protect program integrity and reduce financial leakage.
Out-of-network claim repricing and Independent Dispute Resolution (IDR) workflow optimization — vendor selection, process design, and dispute strategy to maximize savings and minimize provider abrasion under the No Surprises Act framework.
What You Get
Every deliverable is structured, evidence-based, and designed to drive decisions.
Intelligence
Comprehensive evaluations of your PI program across all five dimensions — benchmarked against the market and your peers. Delivered as a detailed report with prioritized recommendations.
Intelligence
We track 170+ vendors across the Payment Integrity ecosystem — capabilities, positioning, competitive dynamics, and market trajectory. Profiles are built from public data, structured operator interviews, and proprietary operational intelligence. Refreshed continuously so what you see reflects the market as it is, not as it was.
Foundation
The foundational session and common classification system that brings clarity and shared language to every PI conversation. Available as a standalone engagement or integrated into any project.
Learn more about PI-Core →How We Deliver
Interactive, facilitated sessions — from PI-Core foundations to deep-dive strategy workshops tailored to your team.
Structured, evidence-based reports with clear findings, benchmarks, and prioritized recommendations.
Ongoing advisory relationships and embedded support for organizations navigating complex PI transformations.
Ready to Talk?